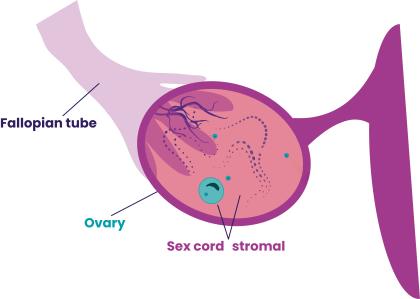
There are many different types of ovarian sex cord stromal tumours (SCSTs). They can be either non-cancerous (benign) or cancerous (malignant). SCSTs develop from the stroma or the sex cord. These are cells in the centre of the ovary that form tissues that support the ovary and help egg cells grow.
Ovarian sex cord stromal tumours are rare. They make up around 7 in every 100 cases of ovarian cancer.
Most ovarian sex cord stromal tumours are diagnosed at stage 1 and treated by surgery alone. If the cancer recurs (comes back), a second surgery may be considered before chemotherapy.
Depending on what types of cells the tumour is made up of, sex cord stromal tumours are divided into:
- Pure stromal tumours: made up of only stromal cells
- Pure sex cord tumours: made up of only sex cord cells
- Mixed sex cord stromal tumours: made up of both stromal and sex cord cells.
Sex cord stromal tumours can behave and respond differently to treatment depending on the specific subtype.
Pure sex cord tumours
- Adult type granulosa cell tumours
Granulosa cell tumours mainly happen in adults. These tumours often produce the hormone oestrogen.
Treatment usually involves surgery to remove as much of the tumour as possible. As the tumours are usually slow growing, they don’t tend to respond very well to chemotherapy.
- Juvenile type granulosa cell tumours
Juvenile granulosa cell tumours are a type of granulosa cell tumour that tend to happen in those under the age of 30, and often in early puberty. These are rare and different from adult type granulosa cell tumours.
If caught at an early stage, the treatment is surgery. For tumours diagnosed at a later stage, surgery may be combined with chemotherapy.
- Other types of pure sex cord tumours
Other types of pure sex cord tumours include:
- Sertoli cell tumour
- Sex cord tumour with annular tubules
Mixed sex cord stromal tumours
- Sertoli-Leydig tumours (androblastomas)
Sertoli-Leydig tumours are a rare sex cord stromal ovarian tumour. Most Sertoli-Leydig cell tumours aren’t cancerous (malignant) and can be removed by surgery.
Sertoli-Leydig tumour cells often produce androgens which include the hormone testosterone. This can lead to virilisation. Virilisation is when a female develops male sex characteristics. This can include a lower pitch of voice, baldness or thicker body hair and pelvic masses (lumps). This happens because the tumour produces the hormone testosterone.
Those who are younger and diagnosed at an early stage may be able to have fertility-preserving surgery. This will allow for the possibility of becoming pregnant later on. You may have additional risk factors to consider and should receive chemotherapy and long-term follow up. You should discuss your individual situation and options with your treatment team.
- Other types of mixed sex cord-stromal tumours
- Sex cord stromal tumour with annular tubules (SCTAT)
- Gynandroblastoma
Pure stromal tumours
- Types of pure stromal tumours
Most pure stromal tumours are non-cancerous (benign). They include:
- Fibroma
- Thecoma
- Fibrosarcoma
- Sclerosing stromal tumour
- Signet ring stromal tumour
- Leydig cell tumour
- Microcystic stromal tumour
- Steroid cell tumour




